Introduction: Individuals with metabolic syndrome or type 2 diabetes are at increased risk of stroke and vascular dementia (1). Currently, little is known about the early drivers of cerebrovascular dysfunction in the context of metabolic disease pathophysiology; however, episodic hyperglycaemia, even in otherwise healthy individuals, may transiently challenge cerebrovascular regulation. Indeed, recent evidence indicates that acute hyperglycaemia may disrupt overall cardiovascular control and impair regulation of arterial blood pressure (ABP) in healthy young adults (2-4). Herein, we hypothesize that acute hyperglycaemia will not only impair regulation of ABP, but also the regulation of cerebral blood flow (CBF) via impairments in the dynamic cerebral blood flow autoregulation (dCA). Confirmation of this hypothesis could shed light on the early mechanisms through which glycaemic disturbances contribute to cerebrovascular dysfunction in metabolic disease.
Objectives: To assess the effects of acute hyperglycaemia on the regulation of ABP and CBF, and on dCA, in healthy young adults.
Methods: Ten healthy young adults (age 28 ± 7 years; BMI 22 ± 4 kg/m²; fasting glucose 4.54 ± 0.41 mmol/L) underwent assessments of blood glucose levels (capillary sampling), CBF, and ABP regulation at baseline and at 30-minute intervals during a 2-hour OGTT (75g). At each time point, hemodynamic parameters were evaluated both at rest and during forced oscillations of ABP induced by a 0.10 Hz paced breathing manoeuvre. CBF was assessed via middle cerebral artery blood velocity (MCAv) using transcranial Doppler (WAKie, Atys Medical), while ABP was continuously recorded using finger photoplethysmography (NIBP, ADInstruments). CBF and ABP regulation were characterized by their respective mean levels and spectral variability (quantified as power spectral density [PSD]) at rest and during forced ABP oscillations in the frequency domain using Fast Fourier analysis. Additionally, dCA was assessed using transfer function analysis between ABP and MCAv. Cerebrovascular responses across the OGTT were analysed using two-way ANOVA. Pearson’s correlation assessed associations between glucose and dCA iAUC.
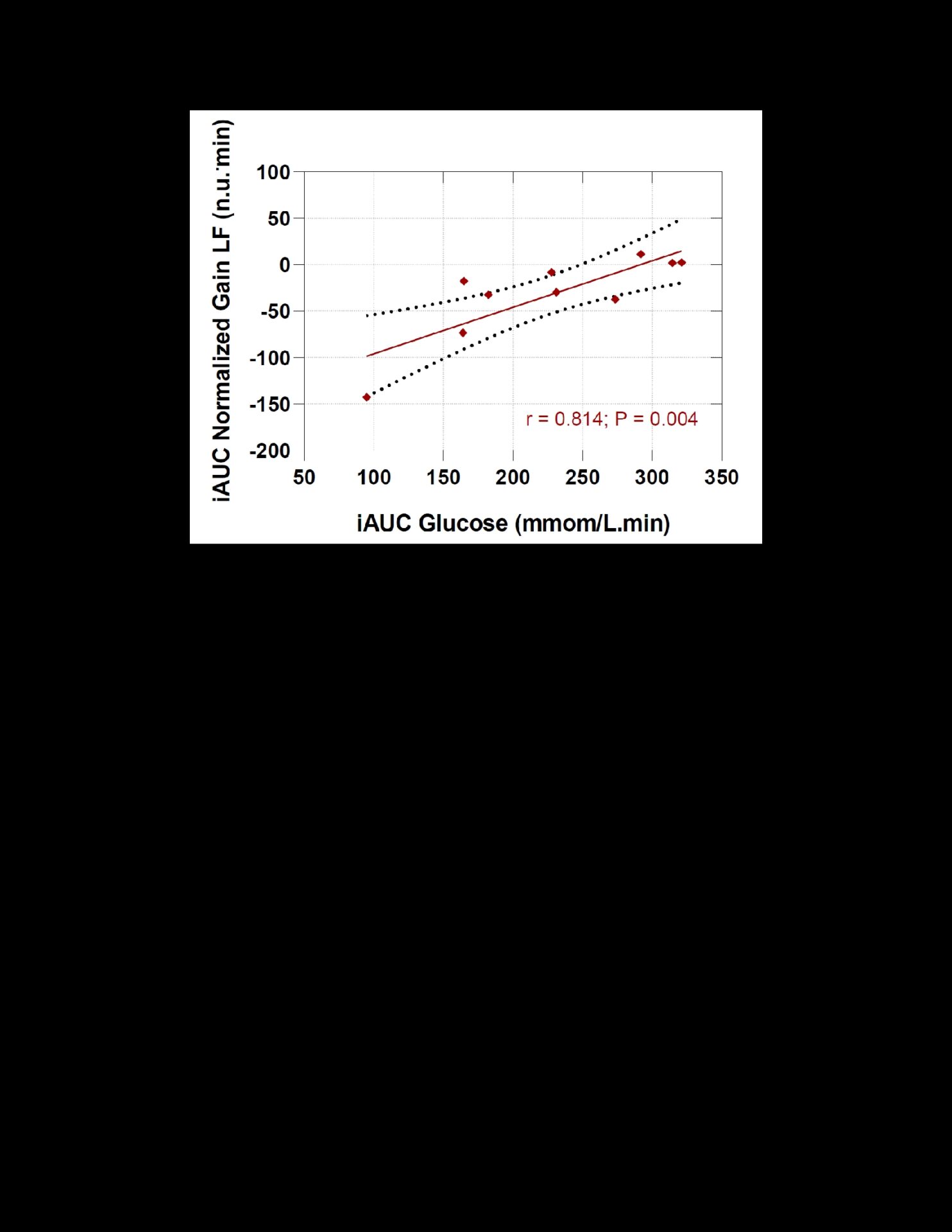
Results: Blood glucose levels increased within the normal range during 2-hour OGTT (iAUC: 227±75 mmol/L·min). Increases in glucose levels during OGTT were accompanied by elevations in mean ABP (baseline = 98±4 vs 120min = 108±6 mmHg, P = 0.002) and ABP variability (baseline = 3.59±0.78 vs 7.20±2.19 mmHg², 120min, P =0.039), confirming that acute hyperglycemia impairs systemic ABP regulation. Despite these changes, there were no detrimental alterations in CBF mean levels, variability or dCA, suggesting that in healthy young adults, cerebral autoregulatory mechanisms maintain stable CBF under hyperglycaemic conditions. However, post-hoc exploratory analyses indicated a trend toward impaired CBF regulation in individuals exhibiting the largest hyperglycaemic responses (r = 0.814, P = 0.004) (Fig.1), suggesting that cerebrovascular control during OGTT-induced acute hyperglycaemia may be altered in individuals with impaired glucose metabolism.
Conclusion: OGTT-induced acute hyperglycaemia may compromise ABP regulation, but cerebral autoregulatory mechanisms appear sufficient to maintain stable CBF in this cohort of healthy young adults. The observed trend between the magnitude of hyperglycaemia and CBF regulation indicates that cerebrovascular responses may be compromised in individuals with impaired glucose metabolism, a hypothesis that warrants further investigations.