Physiology News Magazine
Mental health in academia
An invisible crisis
Features
Mental health in academia
An invisible crisis
Features
Lindsay Bira, Department of Psychiatry, University of Texas Health San Antonio, USA
Teresa M Evans, Department of Pharmacology, University of Texas Health San Antonio, USA
Nathan L Vanderford, Department of Toxicology and Cancer Biology, University of Kentucky, USA
https://doi.org/10.36866/pn.115.32
Everyone has good and bad days. Life throws curve balls and we have quite dynamic responses to them, even when two individuals experience the same event. The diversity of our reactions is on a wide spectrum; depending on the situation and individual. This variation is normal and is driven by many factors. What is not normal is when our reactions become stuck within one of these extremes of unhelpful levels of reaction. When an event or a series of events begin to sequester our emotional real estate, the possibility of the onset or exacerbation of symptoms of anxiety and even depression increase. This is especially true in an already high-stress environment.
Mental health in graduate education is personal for us, as it is for so many who have been a part of academia. We have known faculty as well as trainees who have struggled with their mental health during graduate school, those who struggle currently in their careers, and even several who took their lives along the course of it all. In fact, we have struggled ourselves. We have firsthand experiences with the trials and tribulations of mental health issues, which fuels our passion to address the problem.
Over the last few years, the higher education community has built a better understanding of how impacted some faculty and graduate trainees are by mental health issues given the competitive academic environment. Understanding and addressing mental health in academia is vitally important to support the wellness of our current and future scientific leaders. The key is not crisis response, rather it is in creating a culture of support and prevention – and the time is now.
Mental health issues in faculty
Tragedies such as a suicide have far-reaching impacts, including sparking discussions about mental health. In the academic sphere, the suicides of professors Will Moore and Alan Krueger (Flaherty, 2017; Casselman and Tankersley, 2019) stirred this discussion and highlighted the need for an increased understanding of the impact of mental health on academics. The rates of suicide in academic populations are not clear and data on prevalence of mental health symptoms is limited. That said, Schindler et al. (2006) found that 20% of full-time academic physicians and basic science faculty had significant levels of depression. This was almost equal for males and females, and younger faculty were found to have more emotional distress than their older colleagues. Further, in a cross-institutional survey of 267 US faculty with mental disabilities, mental illness, or symptom histories, nearly 70% had no or limited familiarity with resources available to support their mental health needs, and even fewer used them (13%), mostly due to fear of stigma and professional risk. Respondents indicated that they felt most supported by their spouses or significant others (75% very or extremely supported) and friends (51%) rather than colleagues (29%) and supervisors (25%), though many had not disclosed their mental health needs to their supervisors (Price et al., 2017).
Faculty often highlight the lack of support, high demands, and cut-throat mentalities that lay the groundwork for mental health struggles; they also point out the double-bind of pulling back on workloads or seeking help (e.g., disclosing symptoms or seeking therapy), as there may be personal and professional consequences of addressing the issue at hand. Consequences are a reality whether the decision is to take action or let it lie (Anonymous, 2018a, 2018b; Price et al., 2017). In recent years, professors and academic administrators have used online platforms as well as opportunities to present at national meetings to openly discuss their mental health journeys and suicidal experiences to crack stigma and encourage support (Flaherty, 2015; Knight and Saker, 2016). This is encouraging, as these are essential steps toward building a culture of open discussion for both faculty and graduate students.
Mental health issues in graduate trainees
Mounting data support the fact that graduate trainees face serious mental health challenges. In 2014, the University of California Berkeley Graduate Student Happiness and Well-being Report demonstrated that 43 – 46% of graduate student respondents in the sciences at that institution were depressed (The Graduate Assembly, 2014). The following year, Smith and Brooks (2015), showed that at the University of Arizona, 50% of graduate students surveyed reported “more than average” stress and 23% reported “tremendous” amounts of stress. Levecque et al. (2017) found that 32% of responding Belgium PhD students were at risk of having or developing a common psychiatric disorder. Additionally, Nature’s 2017 PhD survey showed that about 25% of respondents were concerned about mental health and 12% of all respondents sought help for anxiety and depression that was caused by their training program (Woolston, 2017). In these studies, students’ concerns include advisor relationships, career prospects, personal finances, overall wellness (e.g., diet and sleeping issues), living conditions, and their sense of value and inclusion.
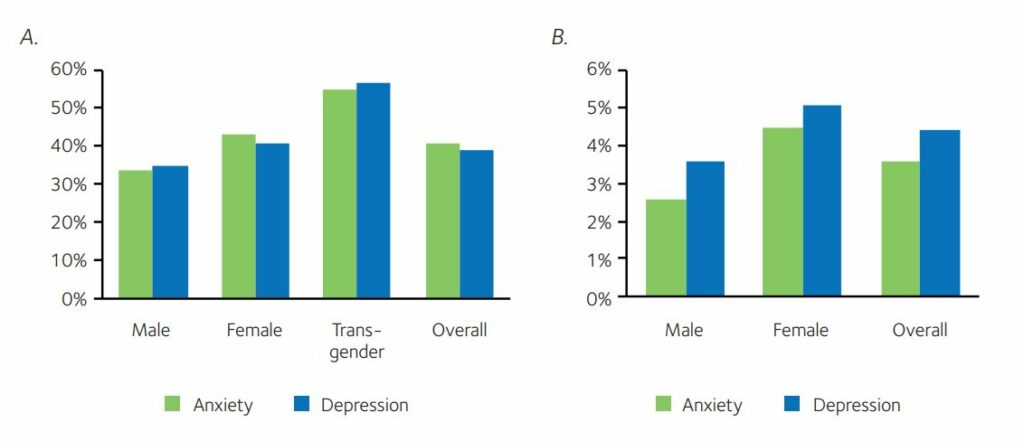
In March 2018, we published an article in Nature Biotechnology further highlighting the critical nature of the mental health issues faced by graduate students. Using the clinically validated scales to assess symptoms of anxiety and depression, General Anxiety Disorder-7 and Patient Health Questionnaire-9, we found that within the context of a cross-sectional, convenience sample of 2,279 graduate students from 26 countries and 234 institutions, 41% had moderate to severe symptoms of anxiety and 39% had moderate to severe symptoms of depression. Female and transgender students showed the highest levels of anxiety and depression symptoms in our study. Positive faculty mentor relationships and a healthy work-life balance were associated with lower symptoms of anxiety and depression (Evans et al., 2018). To put this in context, by comparison the prevalence of anxiety and depression in graduate students is almost an order of magnitude greater than that observed in the general population (see Figure 1) (WHO, 2017).
The stigma of mental health
Stigma around mental health issues is multidirectional, and though much progress toward increasing awareness and access to resources has been made in recent years, much more still needs to be understood and advanced, particularly in high-stress fields. Mental health disorders have been called “invisible wounds” as they are difficult to describe, understand, and see from the outside. They show themselves in disruptive emotional and behavioral patterns, which are unfortunately often attributed to personality flaws, work ethic deficits, underachievement, and health issues.
Misunderstanding and judgment not only come from those viewing the individual, but also from the individual experiencing the symptoms themselves, especially in academic populations. Rigorous training programs select top-tier students who have much of their identity tied up in high performance and achievement. Such identity is greatly challenged during the course of training and into the career span; the demands of academia consistently confront individuals with their own shortcomings, promote unrealistic upward social comparisons, and drive high standards of approval. This easily sets the stage for symptoms of burnout, anxiety, and depression, particularly for those with other known vulnerability factors (e.g., minority status, existing disability, low socioeconomic background, history of trauma or adverse childhood experiences) (Safran et al., 2009; Felitti et al., 1998). When mental health symptoms begin to surface, shame easily develops, particularly when environmental and social support are lacking. Shame drives hiding, denying, and social withdrawal, which complicates symptoms and prevents positive paths forward that could ameliorate mental health issues and their consequences over time.
It is important to note that symptoms do not have to reach the level of a “disorder” or complete dysfunction to be disruptive; many times, a person (especially an academic) is able to “white-knuckle” through symptoms to appear successful in demands and interactions while their internal experience is that of turmoil and exasperation.
If advisors, programs, and institutions do not have procedures in place to appropriately flag, assess, and address such issues using targeted, early-intervention roadmaps, struggling faculty and trainees will continue to fall through the cracks, which can exacerbate existing struggles and potentially build the psychological landscape for suicide risk.
Addressing mental health issues
An essential first step to addressing mental health issues is awareness. Knowing that rates are higher in certain populations gives light to an issue that has previously been undefined or swept aside. Creating more dialogue through research, written features, and social media movements serves to highlight the issue and gives voice to those who are struggling now or who have in the past. Individuals need to know that they are not alone and are valued; organizations need to know that compromised emotional wellness is an understandable reaction to a culture of high stress, and existing mental health disorders are disabilities that require diversity training and inclusion. Just as all entities in the United States are required to have Americans with Disabilities Act-compliant facilities for inclusion purposes, it is important to integrate consistent, accessible, and positively regarded resources for those who begin to suffer or for those with pre-existing mental health disabilities (e.g. major depressive disorder, bipolar disorder, anxiety disorders) to make the academic terrain easier to navigate.
In terms of resources, we propose several. First, training on mental health and emotional wellness should be made available via a variety of modalities for both trainees and faculty. This should focus not only on wellness for the individual but also on how to support others and how to respond to mental health-related events in the department. Second, given that mentorship is an important factor in trainee wellbeing, it is the institutions’ responsibility to ensure that there is specific training focused on effective mentoring practices and modelling wellness for trainees. Third, institutions are at the foundation of establishing a culture that promotes both a sense of community beyond the laboratory or classroom and an expectation ofwellness. Establishing a community wellness culture begins by establishing a clear institutional vision and mission that aligns with the support of trainees, wellness, and community culture. Fourth, it is suggested that anonymous surveys be sent to trainees and faculty to assess mental health; following that, anonymous, digital counseling services should be offered to individuals who flag as symptomatic or at-risk as a gateway to engaging in more intensive counseling (this support model is seen in medical schools such as University of Texas Health San Antonio School of Medicine; Feist, 2018). Lastly, faculty and trainees should be rewarded not only for grants and manuscripts but also for their effective education, mentoring, and wellness practices. Initiatives such as student-driven faculty wellness awards can be a great way to showcase the positive role, modelling that faculty can do to support the institutional culture. Price and Kerschbaum (2017) discuss additional suggestions in their “Resource Guide for Promoting Supportive Academic Environments for Faculty with Mental Illness”.
More research is needed
Research in this area is essential. We need additional data on the prevalence of the range of mental health issues in both faculty and trainees. We also need to understand the root causes of these issues at a much deeper level. There are likely unique and overlapping factors between faculty and trainees that contribute to mental health issues. For faculty, we have a sense that the pressure of winning grants, publishing papers, earning tenure, and promotion are contributing factors. For trainees, career outcome, mentor relationships, and many personal factors play a role. We also need to understand at what point mental health issues arise in faculty and trainees. Do trainees enter graduate school with already elevated rates of mental health issues? Do trainees’ elevated rates of mental health issues carry over into the beginning of a faculty position? Do the rates increase at any particular point in a faculty position or graduate program? To address these questions, there is a clear need to conduct well-controlled population-based longitudinal studies in both faculty and trainees that would study the mental health issues in a cohort of faculty and trainees beginning before they matriculate into the faculty ranks or graduate school and then follow them for some long period of time. Evaluation within such studies should include measures of subjects’ mental health and a multitude of factors that could contribute to changes in their mental health status.
Additionally, some institutions are probably already putting interventions into place that are aimed at addressing the high rates of mental health issues in faculty and trainees. These interventions need to be rigorously evaluated and the findings should be shared with the higher education community. We all need to understand what interventions are being tried and the level of their impact.
Conclusion
Faculty and graduate trainees face a multitude of mental health issues. The shift toward more open discussion and limited research in this area are making this clear. The higher education community needs to better understand the overall prevalence of these issues as well as their causes, and we need to create solutions to fix the problems that are plaguing so many of our current and future scientists. We can no longer stand by, letting this issue continue to cause individuals to suffer alone and be blunted in their personal and professional potential in our fields.
References
Anonymous (2018a). Academia is built on exploitation. We must break this vicious circle. [Online] The Guardian. Available at: theguardian.com/higher-education-network/2018/may/18/academia-exploitation-university-mental-health-professors-plagiarism [Accessed 2 April 2019]
Anonymous (2018b). The invisible injuries of faculty mental health. [Online] Inside Higher Ed. Available at: insidehighered.com/advice/2018/08/31/removing-stigma-faculty-members-mental-health-disorders-opinion [Accessed 2 April 2019]
Casselman B, Tankersley J (2019). Alan B. Krueger, economic aide to Clinton and Obama, is dead at 58. [Online] The New York Times. Available at: nytimes.com/2019/03/18/obituaries/alan-krueger-dead.html [Accessed 2 April 2019]
Evans TM et al. (2018). Evidence for a mental health crisis in graduate education. Nature Biotechnology 36(3), 282 – 4.
Feist JM (2018). Dear doctor, get well soon. [Online] Mission Magazine, UT Health San Antonio. Available at magazines.uthscsa.edu/mission/dear-doctor-get-well-soon/ [Accessed 10 May 2019]
Felitti VJ et al. (1998). Relationship of childhood abuse and household dysfunction to many of the leading causes of death in adults. American Journal of Preventive Medicine 14(4), 245 – 58.
Flaherty C (2015). Personal philosophy. [Online] Inside Higher Ed. Available at: insidehighered.com/news/2015/02/25/professors-reflections-his-battle-depression-touch-many-recent-disciplinary-meeting [Accessed 2 April 2019]
Flaherty C (2017). Aftermath of a professor’s suicide. [Online] Inside Higher Ed. Available at: insidehighered.com/news/2017/04/21/recent-suicide-professor-sparks-renewed-discussions-about-access-mental-health [Accessed 2 April 2019]
Knight C, Saker A (2016). For Ono, the time to speak about mental health is now. [Online] Cincinnati.com. Available at: cincinnati.com/story/news/2016/05/22/santa-ono-breaks-silence-mental-illness-suicide/84733466/ [Accessed 2 April 2019]
Levecque K et al. (2017). Work organization and mental health problems in PhD students. Research Policy 46(4), 868- – 79.
Price M et al. (2017). Disclosure of mental disability by college and university faculty: the negotiation of accommodations, supports, and barriers. Disability Studies Quarterly 37(2). DOI: 10.18061/dsq.v37i2
Price M, Kerschbaum S (2017). Promoting supportive academic environments for faculty with mental illnesses: resource guide and suggestions for practice. [Online] Temple University Collaborative. Available at: tucollaborative.org/wp-content/uploads/2017/05/Faculty-with-Mental-Illness.pdf [Accessed 10 May 2019]
Safran MA et al. (2009). Mental health disparities. American Journal of Public Health 99(11), 1962 – 6.
Schindler BA et al. (2006). The impact of the changing health care environment on the health and well-being of faculty at four medical schools. Acad Med 81(1), 27 – 34.
Smith E, Brooks Z (2015). Graduate student mental health 2015. [Online] University of Arizona: National Association of Graduate-Professional Students Institute. Available at: nagps.org/wordpress/wp-content/uploads/2015/06/NAGPS_Institute_mental_health_survey_report_2015.pdf [Accessed 2 April 2019]
The Graduate Assembly (2014). Graduate student happiness & well-being report | 2014. [Online] UC Berkeley. Available at: ga.berkeley.edu/wp-content/uploads/2015/04/Well-Being-Report-Deck.pdf [Accessed 2 April 2019]
WHO (2017). Depression and Other Common Mental Disorders: Global Health Estimates. Geneva: World Health Organization.
Woolston C (2017). Graduate survey: a love-hurt relationship. Nature 550, 549 – 52.
