Physiology News Magazine
What makes a good night’s sleep?
The external and internal factors that influence a good night’s sleep
Features
What makes a good night’s sleep?
The external and internal factors that influence a good night’s sleep
Features
Ciro della Monica and Derk-Jan Dijk, Surrey Clinical Research Centre and Surrey Sleep Research Centre, University of Surrey, UK
https://doi.org/10.36866/pn.113.36
We all experience good and bad nights of sleep, and we know that if we don’t sleep well this profoundly impacts our mood, alertness, productivity, health and well-being. But what is it that defines a good night’s sleep and is this the same for everyone? We briefly explore the physiology of sleep and how it is regulated, the aspects of sleep that contribute to sleep quality and brain health, and the factors (internal and external) that put our sleep at risk.
What is sleep and how is it regulated?
The phenomenology of sleep
The definition of sleep as “a reversible behavioural state of perceptual disengagement from, and unresponsiveness to, the environment” (Carskadon & Dement, 2011) captures some of the essential differences between wakefulness and sleep. During wakefulness we actively interact with our environment, and are conscious of our surroundings and ourselves. During sleep this consciousness ceases, except for when we dream.
Moving from wakefulness to sleep and dreaming is associated with changes in brain activity (Fig. 1).

During wakefulness brain waves are fast with a low amplitude. When we enter sleep the frequency of brain waves becomes progressively slower and their amplitude increases. This part of sleep is classified into three different stages (N1, N2, and N3), with N3 often considered “deep” sleep and called slow-wave sleep (SWS).
The N refers to non-Rapid Eye Movement sleep (NREM), because, unlike in wakefulness, there are no rapid eye movements in this sleep state. After a first episode of NREM we enter Rapid Eye Movement (REM) sleep.
The brain activity during this state is somewhat similar to wakefulness and, as the name suggests, there are rapid eye movements even though the eyes are closed. REM sleep is further characterised by muscle atonia, and when we wake up from REM sleep some of us will, for a short period, feel paralysed and often remember our dreams. During a normal night of sleep there will be four to five cycles of NREM-REM sleep, each lasting 90 – 120 min (Fig. 2).
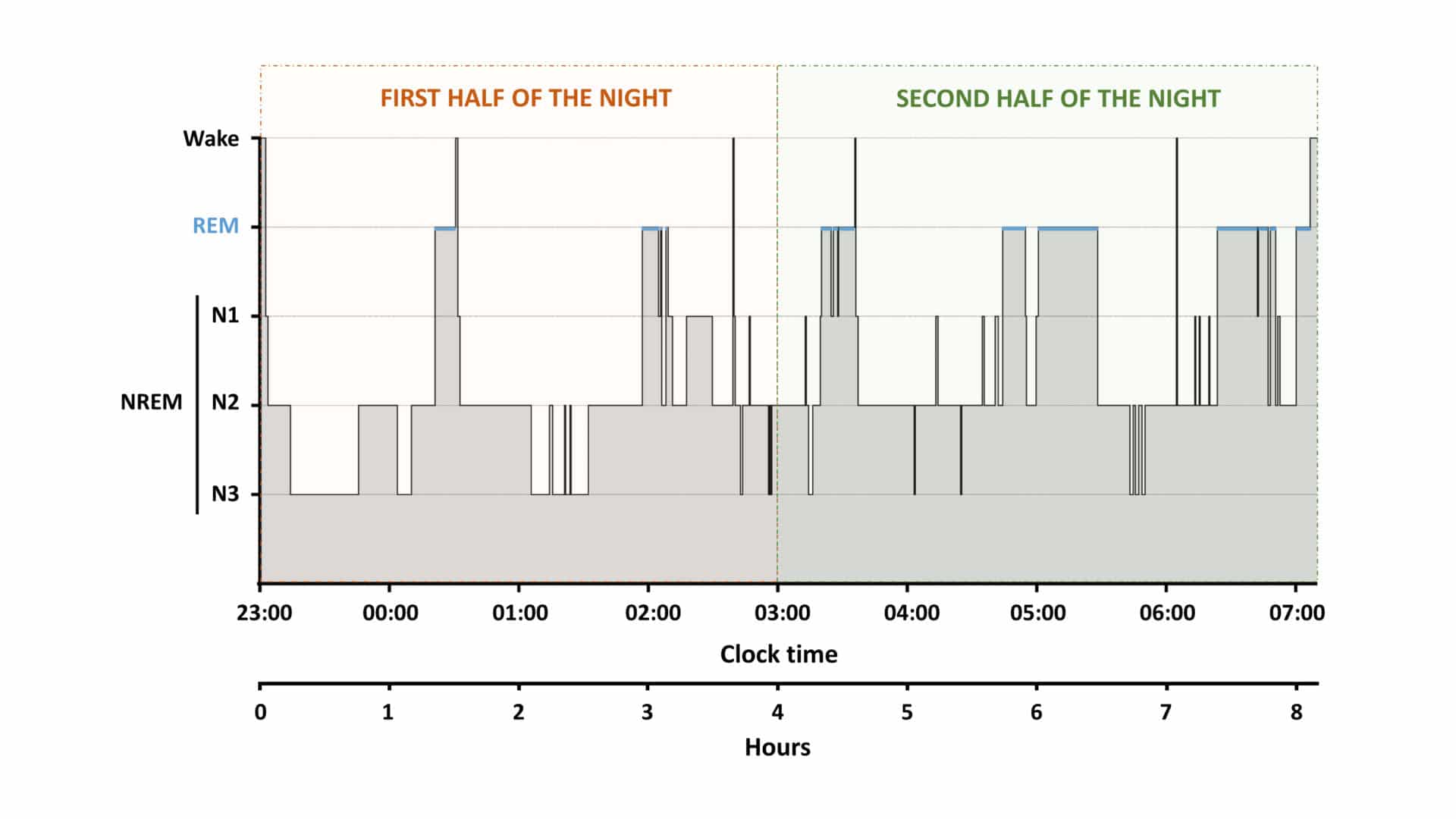
The content of the cycles changes as the night progresses. Initially there is much SWS while REM periods are short; later on there will be less and less SWS with REM periods becoming longer. Both NREM and REM sleep are interrupted repeatedly by short periods (half a minute or slightly longer) of wakefulness because, for example, we move or hear a sound. In one night there may be several very short awakenings, very few of which we will remember (e.g. 16 objective vs. 2 subjective median awakenings, della Monica et al., 2018). Brain activity, muscle tone, and eye movements are not the only variables that change across wakefulness, NREM, and REM sleep. Heart rate, hormones, body and brain temperature are all affected and exhibit predictable changes.
The regulation of sleep
The timing of sleep and the typical phenomenology of a night’s sleep are regulated by two processes (Borbély, 1982) (Fig. 3).

The first process, referred to as a homeostatic process (Process S), essentially monitors time awake with sleep debt increasing during wakefulness and dissipating during sleep. The progressive reduction in SWS in the course of a night of sleep and the increase in SWS following sleep deprivation is thought to reflect this homeostatic process.
The second process is the circadian process (Process C). The circadian pacemaker located in the hypothalamus drives ~24-hour rhythms in physiology and behaviour including a rhythm in sleep-wake propensity. The circadian drive for wakefulness increases progressively during the day, peaks during the early evening hours and then suddenly subsides at the beginning of the night, at around the time of the onset of secretion of the hormone melatonin. Later in the night, the circadian process actively promotes sleep, particularly REM sleep.
Thus, during the day, the wake-dependent increase in homeostatic sleep drive is countered by the progressive increase in the circadian drive for wakefulness. During the night the homeostatic dissipation of sleep propensity is countered by the circadian increase in sleepiness. Under normal conditions, when we work during the day and sleep at night, these two processes combine to produce consolidated episodes of daytime wakefulness and nocturnal sleep (Dijk & Czeisler, 1994). Taking these two processes into account and knowing that the circadian process is rather inert, i.e. cannot be shifted easily, it is easy to understand why shift workers struggle to sleep during the day and to stay awake at night.
Over the years, many experiments have confirmed the predictions of the two-process model and new aspects have been discovered. For example, it has been demonstrated that sleep homeostasis is to some extent regional and use-dependent. Thus, the build-up and dissipation of Process S is fastest in those areas of the brain which have been most active during the day. Furthermore, hypotheses about the neurochemical and neuronal basis of the sleep homeostatic process have been proposed. The “adenosine” hypothesis of sleep regulation states that neuronal activity is associated with the release of adenosine, which then binds to adenosine receptors and makes us sleepy. When we drink coffee to stay awake we make use of this system because caffeine blocks adenosine receptors. The “synaptic homeostasis hypothesis of sleep function” proposes that during wakefulness when we interact with the environment and much information enters our brains, connections between neurons (synapses) become stronger and larger. This cannot go on forever because our brain has limited space. Therefore it is thought that during sleep the overall synaptic strength is rebalanced (Tononi & Cirelli, 2014).
Genetic variation in the generation of circadian rhythms and in the speed of our clocks have also been identified (Zhang et al., 2011). If your genetic makeup makes your circadian clock tick fast you will be a morning type (i.e. “early bird”), whereas a genetically slow ticking clock will make you an evening type (i.e. “night owl”).
However, you cannot blame everything on your genetic circadian make-up. Behavioural choices, such as how much artificial light we consume in the evening, have a profound influence on the circadian clock and our ability to get up in the morning (Skeldon et al., 2017).
What does good and bad sleep really mean?
Sleep quality can be assessed both subjectively, through completion of questionnaires (“how well did you sleep?”) and objectively, through polysomnography (PSG) i.e. measurement of brain waves, muscle tone, eye movements, blood oxygen levels, movements of limbs etc. during sleep.
Objective vs. subjective quality of sleep
From PSG data, objective parameters such as total sleep time, % time spent in each sleep stage, time to fall asleep (sleep onset latency), sleep efficiency, and number of awakenings during the night can be derived. You can then determine which objective parameter best correlates with the subjective experience of sleep.
We assessed the sleep of 206 healthy men and women (20 – 84 years old) without sleep complaints (della Monica et al., 2018). After controlling for the age- and sex-related changes in sleep, we found that while inter-individual variations in SWS (deep sleep) could not predict subjective sleep quality, two other PSG-derived variables could. A large number of night awakenings (NAW) was associated with reports of poor quality sleep. Longer duration of REM sleep correlated with self-reported good sleep quality and how refreshed people felt upon awakening. Interestingly, the associations between objective sleep variables and subjective sleep quality was much stronger in women than men, and was consistent across the whole age range studied.
Another large scale study in 1483 older adults (≥65 years) (Kaplan et al., 2017) also reported that sleep continuity-related measures are an important determinant of subjective sleep quality, although in this study the role of REM sleep was not so clear. However, a recent comparison of patients with primary insomnia and good sleepers found that the patients spent significantly less time in REM (Baglioni et al., 2014) supporting the notion that REM sleep is important for sleep quality.
Objective sleep quality: Association with brain function
We may also want to know which aspects of sleep contribute to objective brain functioning or brain health. There are many aspects to brain function: alertness, mood, attention, working memory, long-term memory, speed of response, creativity, ability to plan ahead, ability to shift from one task to another, etc. These can be assessed by a wide variety of performance tests and questionnaires, and many of these aspects of brain function change with age, some more than others.
To reduce the enormous amount of variables, data reduction approaches such as factor analysis can be used. In one such approach, we assessed 51 performance variables and reduced these to four factors, the most important three of which were: mood/alertness, response time, and accuracy (della Monica et al., 2018). With age we become more alert, and our mood is more positive. Our response times become slower but we maintain accuracy. Assessment of the independent contribution of objective sleep parameters showed that more slow wave sleep predicted faster response times. Fewer awakenings and more REM sleep were associated with maintained accuracy. These observations were made in healthy people without signs of more than normal age-related cognitive decline. Other studies have shown that sleep continuity and REM sleep are protective against more severe cognitive decline and the development of dementia (see della Monica et al., 2018 for references). Sleep disorders, such as sleep disordered breathing, also contribute to cognitive decline. The mechanisms through which normal sleep and sleep disorders contribute to brain function remains unknown. However, some researchers have suggested that sleep contributes to brain health through clearing of toxic or harmful metabolic by-products from the brain.
Which external and internal factors can impact the quality of our sleep/wake cycle?
The bedroom environment can have a profound impact on the quality and quantity of sleep. Noise and low and high temperatures are often cited as reasons for poor sleep. In a survey of 1375 individuals in Switzerland, self-reported sleep quality was linked to annoyance by nocturnal traffic noise (Frei et al., 2014). In a Norwegian survey of 2898 participants, a positive relationship was found between exposure to traffic noise and psychological distress symptoms in those with poor sleep quality, suggesting these individuals may be more vulnerable to the effects of traffic noise (Sygna et al., 2014). An analysis of 765,000 US survey respondents (2002–2011) and nocturnal environmental temperature information demonstrated that increased temperatures at night are associated with elevated self-reports of insufficient sleep particularly in summer and in older individuals (Obradovich et al., 2017). This suggests that climate change may impact sleep, and our hot and noisy cities don’t make for a good sleeping environment.
Light is another physical environmental factor that is known to affect sleep. Moonlight and the full moon have been thought to disrupt sleep but recent studies in the laboratory (della Monica et al., 2015) and at home (Haba-Rubio et al., 2015) have failed to support this notion. There are more and more sources of biologically effective artificial light. LEDs and screens from smart phones/tablets emit light which often has a high blue light content. Artificial evening light can slow down our clock making us think that it is not yet time to go to bed. Light has also direct alerting effects; in other words, makes us less sleepy at any time of day. Just like drinking coffee later in the day, consuming too much light in the evening will keep you awake and, alongside frequent texting and internet activities, will make it difficult to switch off.
In fact, not being able to switch off and worries about work and family are among the most commonly cited internal reasons for poor sleep. Maybe this is not surprising, but it nevertheless shows that besides biological processes, such as sleep pressure and circadian rhythmicity, and external environmental factors, there are cognitive or psychological factors that have a profound impact on sleep quality. Importantly, these biological and non-biological factors interact. This is well illustrated by cognitive behavioural therapy for insomnia, of which a central component of this multicomponent therapy is sleep restriction. Limiting sleep increases homeostatic sleep pressure, makes you fall asleep more quickly, and thereby helps the patient to disengage from those internally generated worries.
Conclusion
Recent research confirms the importance of good quality sleep and has identified some of the key aspects of sleep contributing to subjective and objective sleep quality. It has identified factors that may jeopardise a good night’s sleep and simple changes to our environment and lifestyle that can be made to improve sleep.
References
Baglioni C, Regen W, Teghen A et al. (2014). Sleep changes in the disorder of insomnia: A meta-analysis of polysomnographic studies. Sleep Medicine Reviews 18, 195–213.
Borbély AA (1982). A two process model of sleep regulation. Human Neurobiology1, 195–204.
Carskadon MA, Dement WC (2011). Normal Human Sleep: An Overview, in: Principles and Practice of Sleep Medicine. Elsevier Saunders, St. Louis, 16–26.
della Monica C, Atzori G, Dijk D-J (2015). Effects of lunar phase on sleep in men and women in Surrey. Journal of Sleep Research 24, 687–694.
della Monica C, Johnsen S, Atzori G et al. (2018). Rapid eye movement sleep, sleep continuity and slow wave sleep as predictors of cognition, mood, and subjective sleep quality in healthy men and women, aged 20–84 years [Online]. Frontiers in Psychiatry 9, 255. DOI: 10.3389/fpsyt.2018.00255
Dijk D-J, Czeisler CA (1994). Paradoxical timing of the circadian rhythm of sleep propensity serves to consolidate sleep and wakefulness in humans. Neuroscience Letters 166, 63–68.
Frei P, Mohler E, Röösli M (2014). Effect of nocturnal road traffic noise exposure and annoyance on objective and subjective sleep quality. International Journal of Hygiene and Environmental Health 217, 188–195.
Haba-Rubio J, Marques-Vidal P, Tobback N et al.
(2015). Bad sleep? Don’t blame the moon! A population-based study. Sleep Medicine 16, 1321–1326.
Kaplan KA, Hirshman J, Hernandez B et al. (2017). When a gold standard isn’t so golden: Lack of prediction of subjective sleep quality from sleep polysomnography. Biological Psychology 123, 37–46.
Obradovich N, Migliorini R, Mednick SC et al. (2017). Nighttime temperature and human sleep loss in a changing climate [Online]. Scientific Advances 3(5), e1601555. DOI: 10.1126/sciadv.1601555
Skeldon AC, Phillips AJK, Dijk D-J (2017). The effects of self-selected light-dark cycles and social constraints on human sleep and circadian timing: a modeling approach [Online]. Scientific Reports 7, 45158. DOI: 10.1038/srep45158
Sygna K, Aasvang GM, Aamodt G, Oftedal B, Krog NH (2014). Road traffic noise, sleep and mental health. Environmental Research 131, 17–24.
Tononi G, Cirelli C (2014). Sleep and the price of plasticity: from synaptic and cellular homeostasis to memory consolidation and integration. Neuron 81, 12–34.
Zhang L, Jones CR, Ptacek LJ, Fu Y-H (2011). The Genetics of the Human Circadian Clock, in: Advances in Genetics. 231–247.
